Blog

Powerful Benefits of Chiropractic Care for Sports Athletes
Playing sports on a competitive or semi-competitive level is extremely demanding on your body. Your muscles are required to push and pull at your maximum

Back to Basics: Sleep Hygiene
Your circadian rhythm is your, “sleep/awake cycle,” it is a 24 hours cycle your body goes though with sleep and being awake. Regulating your rhythm

What Causes Inflammation?
Bottom Line: Chronic inflammation is one of the most significant health issues many of us will face today. It’s been linked to everything from chronic
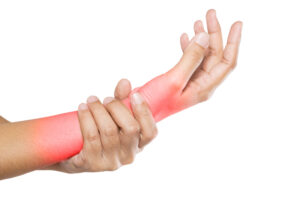
Is My Hand Pain Carpal Tunnel?
Carpal tunnel is a diagnosis that often gets blamed for all hand and finger pain. But what is carpal tunnel? Lets start this journey at

Back to Basics: Organic vs Non-Organic Foods
What is organic agriculture? The International Federation of Organic Agriculture Movements defines organic agriculture as, “a production system that sustains the health of soils, ecosystems
Can Chiropractors Help With…
This is a question we get a lot. Can Chiropractic care help with (insert random pain here)? If you fill the blank with a cause
In Pain? Need Treatment?
Simply give us a call or book an appointment online. Our professional team of chiropractors will take a closer look to suggest the best treatment for your needs. We are here to help!
